WHAT IS ACUTE PAIN: the basics of pain science
Part 1 in understanding how your body interprets pain.
Written by Resilient Health Osteopath Dr Mel Pierlot.
If you are reading this blog, you are probably experiencing pain right now, or you know someone who is suffering with it.
You will probably know how debilitating it can be in the way it interferes with your:
work
social life
hobbies
sleep
personality
and the frustration that might occur with relapses (both yours and those close to you)
Wherever you are in your pain journey, great work!
You have made the right step in reading up more about pain. Knowledge is absolutely power when it comes to pain; the more you understand pain, the more tools you will have to help manage and overcome it.
This blog will explain the basics of pain science so that when you are in the thick of it, you can embrace your pain, rather than shy away from it.
This blog will be about ACUTE pain which is pain lasting up to 3 months or within the expected tissue healing time frame.
The official definition of PAIN is an ‘unpleasant sensory and emotional experience associated with actual or potential tissue damage’- this is a great place to start because it already tells us so much about what pain is.
Let’s break it down into parts:
1. ‘Sensory’:
Pain is a sensation in the same way that heat, cold, pressure and vibration are. It is merely information that the brain receives about what is happening in your body.
Here is a very basic flow chart to describe how pain signalling works (which is the same as the other sensations!):
*If you dont' know what stepping on a piece of lego feels like... think of a stone... please do not attempt to cause harm or pain at home.

A very key component of this chart is that pain is not felt until after the brain interprets the information. This means that it is up our brain whether we feel pain or not.
For example, if you step on a piece on a piece of Lego JUST after you’ve cleaned up the house, you’re probably going to feel pain, and be pretty ticked off too. But if you step on a piece of Lego in a home invasion situation, you are probably not going to feel that pain until you’re finally resting safely at your friends place.
Your brain will decide when it is important for you to know about pain.
Does this mean that ‘pain is all in your head’? Yes and no.
Even though pain is up to your brain, it is still a very real sensation and experience.
2. 'Actual or potential tissue damage’:
Pain is a wonderful adaptation and is vital for our biology and survival. Pain is our protector!
Without pain we wouldn’t know if we had an injury or infection that could endanger our wellbeing.
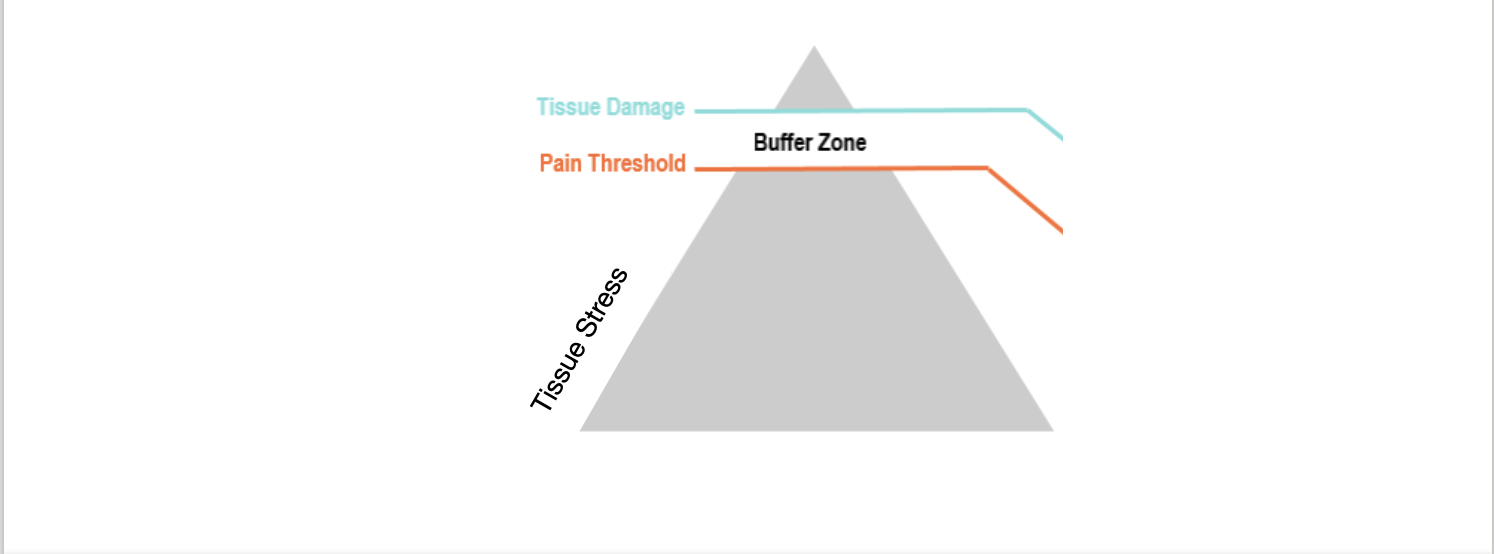
Here is a picture demonstrating how pain is our protector. Our brain will trigger the pain response well before there is actual damage to protect our tissues. In the example of stepping on a piece of lego (tissue stress), our brain will give us the sensation of pain in the skin (pain threshold) before the lego piece actually breaks the skin and reaches muscles/ nerves/ bones (tissue damage)
This is important because it shows us that pain is protective and that pain does not always mean damage.
3. ‘Emotional’:
A frequently overlooked piece of the pain puzzle is the connection between emotions and pain.
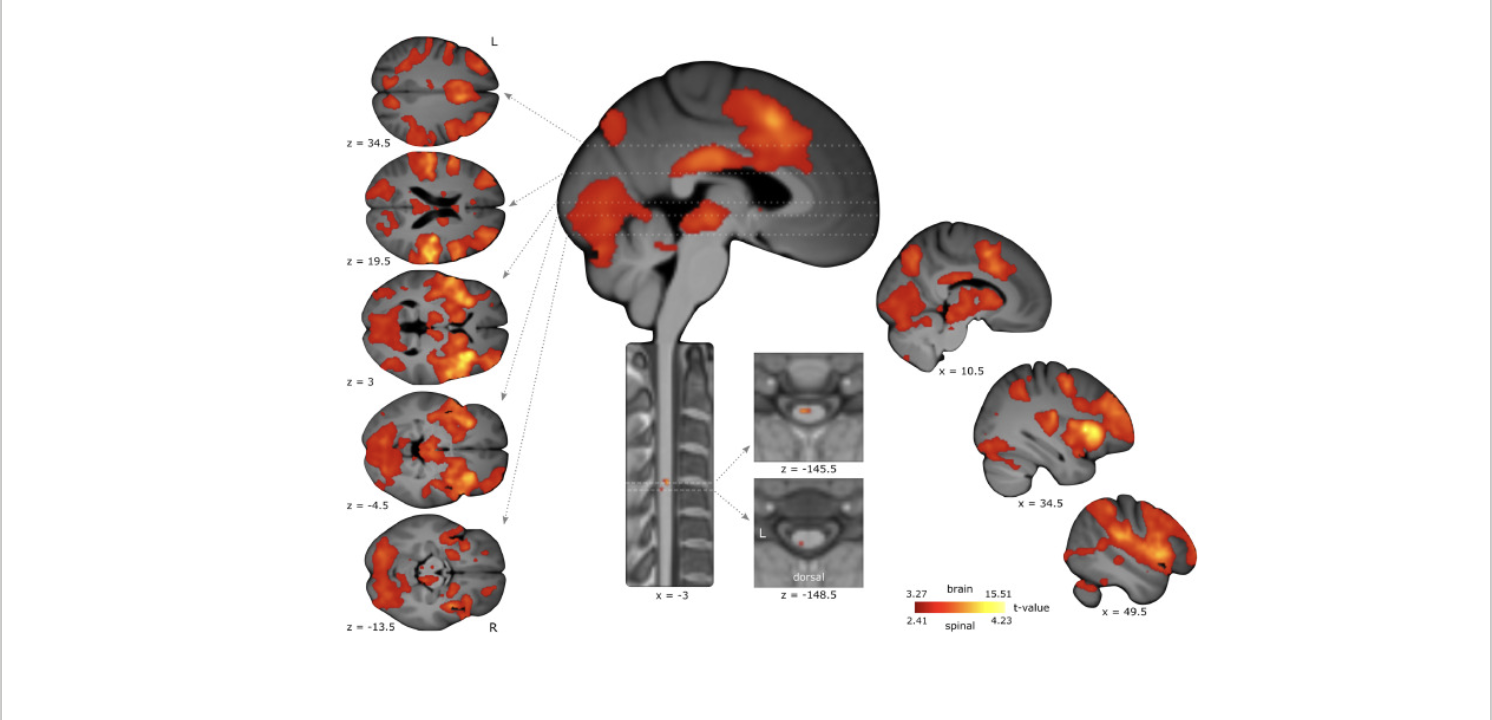
Here is an image of brain activity while in pain. If pain was just a sensation, then only one part of the brain would be active. But what we can see here is that many parts of the brain are involved in the processing and perception of pain!!
In this image, we can see that the parts of the brain that control our senses, mood, decision making, memory, learning, stress and fear are also active when we are in pain!
This explains why sometimes you don’t feel like yourself when you’re in pain. This also means that your stress, fear and mood can impact how your brain perceives (and therefore feels) pain, AND that your brain has the ability to learn and remember pain.
In Conclusion...
Understanding pain science can feel overwhelming.
The biggest takeaways from acute pain science is that:
- Pain is our protector
- Pain does not always mean damage
- Pain is emotional and emotions affect pain
See you in the clinic!
The Resilient Health Team
References
International Association for the Study of Pain. (2020, July 16) IASP Announces Revised Definition of Pain. https://www.iasp-pain.org/publications/iasp-news/iasp-announces-revised-definition-of-pain/
Moore, K., Agur, A. and Dalley, A., 2014. Clinically oriented anatomy. 7th ed. Lippincott Williams & Wilkins
Pain Revolution. (n.d.). The Key to Understanding Pain. https://www.painrevolution.org/factsheets
Tinnermann, A., Büchel, C., & Cohen-Adad, J. (2021). Cortico-spinal imaging to study pain. NeuroImage, 224, 117439.
doi.org/10.1016/j.neuroimage.2020.117439
Yang, S., & Chang, M. C. (2019). Chronic Pain: Structural and Functional Changes in Brain Structures and Associated Negative Affective States. International journal of molecular sciences, 20(13), 3130. doi.org/10.3390/ijms20133130
IMAGES:
Image 1: created by Dr Mel Pierlot (Osteopath)
Image credit 2: https://www.hingehealth.com/blog/movement-is-medicine/
Image credit 3: https://www.sciencedirect.com/science/article/pii/S1053811920309241
