I’VE HURT MY BACK, NOW WHAT?!?
Written By Our Resident Resilient Health Chiropractor, Dr Stewart Ward D.C
You’re at the gym, pushing some heavy steel.
You’re bending over to pick up your child, or carry all those groceries to the car.
You’ve been out in the garden for hours - weeding, digging, green-thumbing it up.
You let rip with the biggest sneeze of your life...
SNAP! CRACKLE! POP! PAIN!
As Wash from Firefly would say:

You’ve hurt your back; an injury has occurred and now you want to know what to do:
Keep Calm & Carry On
Alrite, first things first - let’s just sloooooooow down & just breathe.
If you’ve ever played sports or even just stepped off a curb and rolled your ankle, you wouldnt freak it - you’d be filthy, but you wouldnt freak out. It’s just a rolled ankle!
Walk it off!

There is a tendency to panic and "freak out" when it comes to our spine...
It must be really serious, I’m in so much pain!!
Because our spine houses our nervous system, the immediacy and intensity of that pain can really drive us to think it’s a serious injury. The neuro-circuitry is designed this way, to ensure that we do not continue to place ourselves in immediate "DANGER". However, sometimes our brain's interpretation of this after the immediate instance needs a little help.
You see, alot of the time it can be just like that rolled ankle - the joint was put into a position it didnt like or couldnt control and there’s pain as a result. Encouraging us to let the joint have a moment, to recalibrate.
However just to be sure - let’s go the scary stuff check list shall we?
1. Does it hurt if you cough, sneeze or swallow?
2. Is there any change to your bladder or bowel function? Feeling like you’re not going to make it to the bathroom in time?
3. Is there any numbness or altered sensation in the region of your genitals?
If any of the above answers were yes, especially around bladder and bowel function and sensation, this can be a sign of something called Cauda Equina and this can be a serious, life threatening medical condition.
Even if you came to visit us, we would be sending you to the ER for immediate checks.
So...
NOW that we’ve established that at least for now, this isnt a serious issue so we can focus on the first thing
-> settling down some pain.
All you need is LOVE
A great way to do this, is to change how your brain is feeling about this area by giving it different inputs.
That could be going for little walks (even just for a minute around the house), taking some nice deep breaths or using heat &/or ice.
We can also try and protect the area when we go to move by actively tensing our trunk muscles (Front & back) to add some extra stiffness to the area.
Another way we like to change up signal, is by developing an awareness for supporting the injured area by propping a pillow under or between knees when we are trying to sleep:
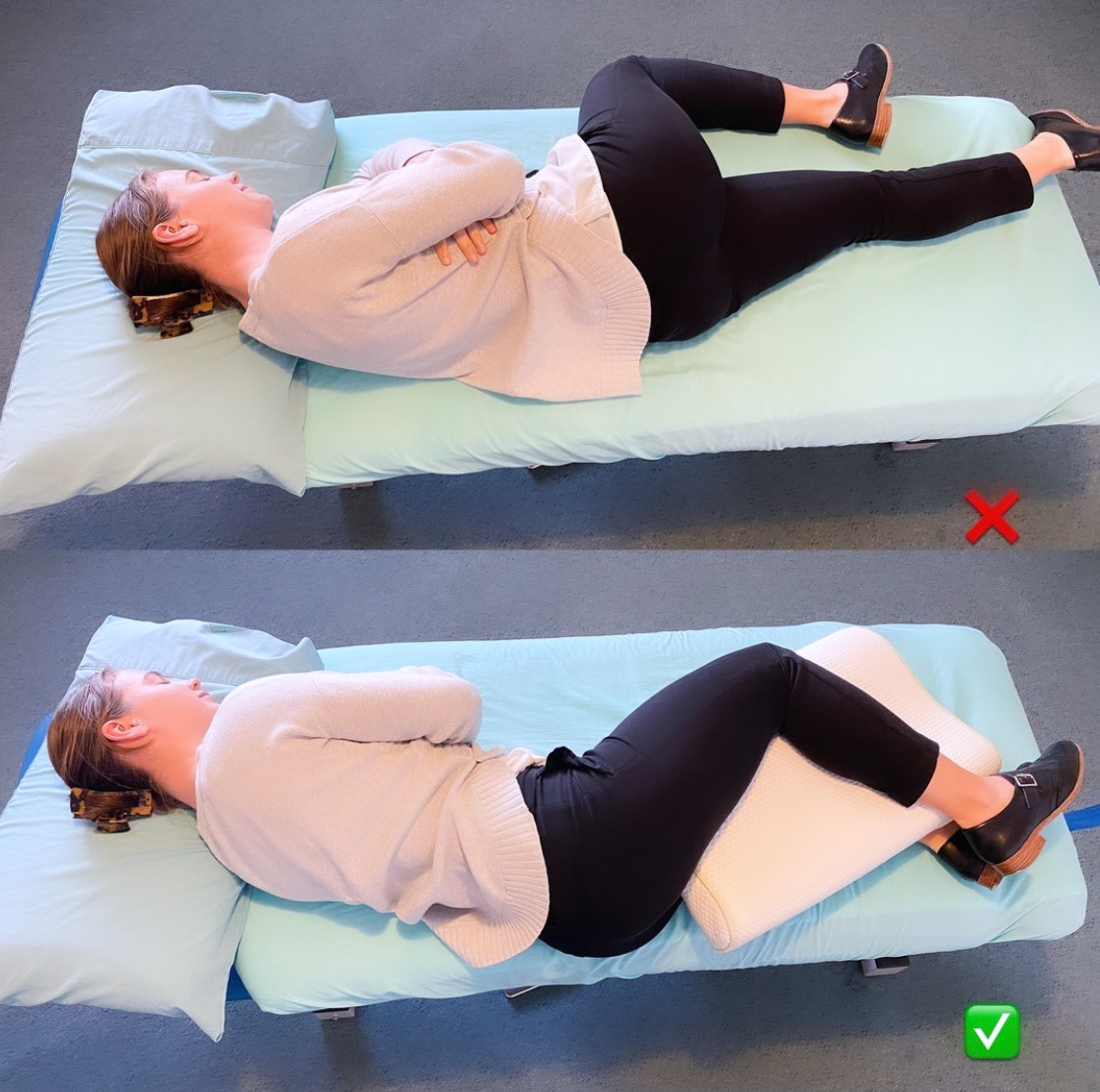
And checking in with how we stand:
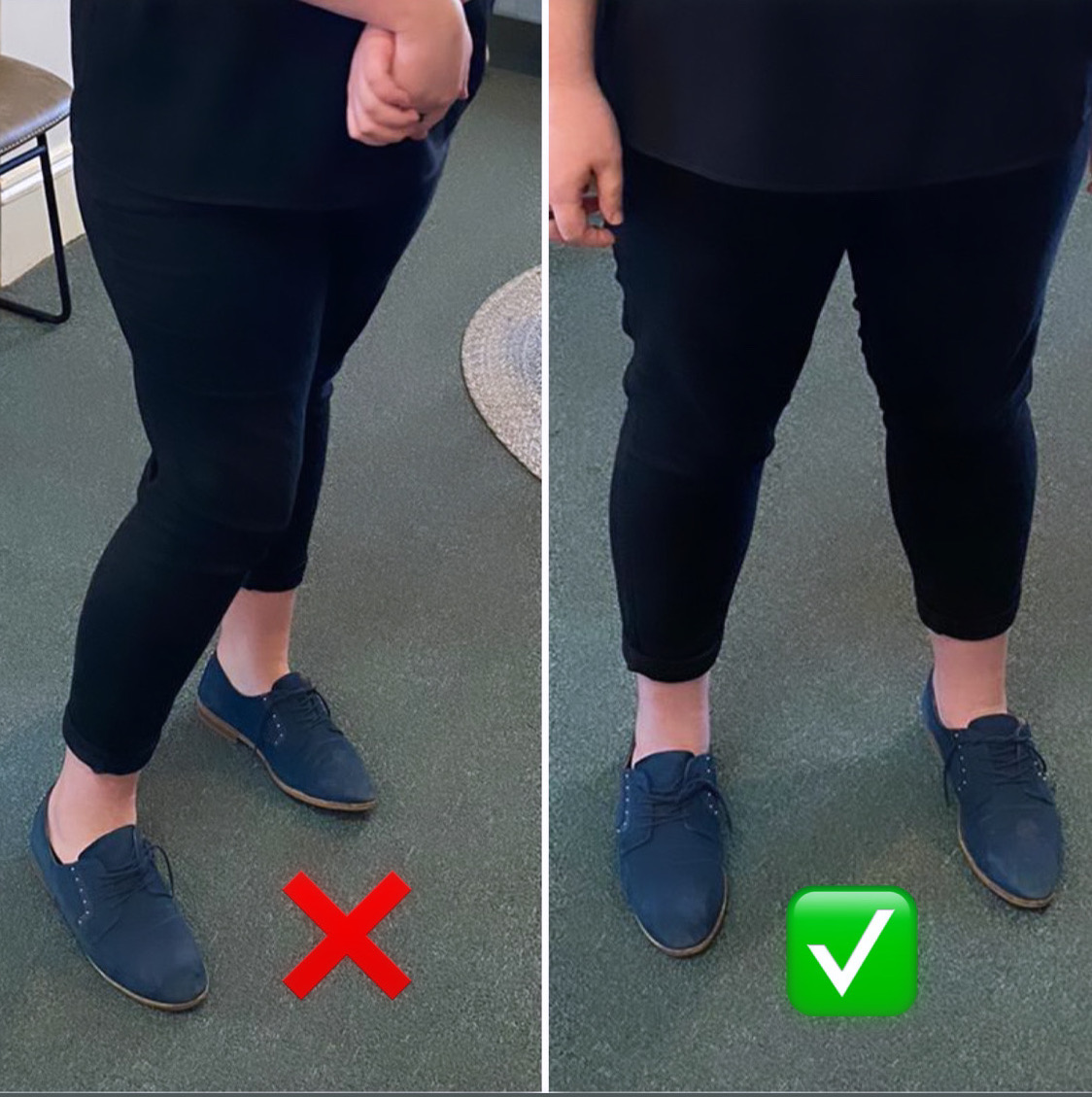
How do you do this you ask?
Well, here you go:
- Tense your abdominal muscles (stick some fingers into your stomach and push them away, not sucking in)
- Tense your side abdominals/obliques (imagine fingers poking into your sides, and pushing them out)
- Tense/squeeze your big back muscles
- Engage your lats and serratus (your side body!) by imagining you’re trying to squash an soft drink can in your armpits
Here is our video showing you how to do this standing:
You can also check out this link:
Frequently Asked Questions:
ICE OR HEAT?!
We get this one all the time! The answer is - whichever one you like!
The old-school answer was ice, because we were trying to limit inflammation. But inflammation is also the first phase of injury healing, so that seems kinda silly?
Fun Fact - did you know the man who wrote the study on using ice to reduce inflammation recanted his statement in 2017 & was official removed from recommendations in 2019?
Speaking of managing inflammation….
ANTI INFLAMMATORIES & PAINKILLERS
The British Journal of Sports Medicine (BJSM) put out an updated version R.I.C.E (Rest, Ice, Compression, Elevation) in 2019 called PEACE & LOVE
In it, the A stood for AVOID ANTI INFLAMMATORIES. Again, inflammation is the first phase of healing so we want to try to avoid them if possible - studies have shown poor effectiveness when it comes to both acute and chronic low back pain as well as long term use been linked to stomach dysfunction.
Painkillers such as a paracetemol (think Panadol, Panamax etc) are ok in the short term, especially if they help get sleep.
SHOULD I GET A MASSAGE?
This can sometimes be a personal preference, but generally speaking in the literature massage has shown poor evidence in regards to helping with acute low back pain episodes.
It may end up been lot of short term pain to massage an injured area without any demonstrable benefit.
Seek Advice
So you’ve done the checklist, made sure this is a serious injury and have done some self care to help calm stuff down. What next?
This is a great time to book in!
Things have hopefully calmed down, so a thorough examination can be performed to determine the cause and extent of the injury, provide treatment and education to help you with pain management, and to collaborate on a management plan specifically tailored to you to help you get out of pain and get back to doing what you love.
Early treatment involving adjustments and/or manipulation has been shown in the literature to have a strong evidence for helping with both acute and chronic low back pain cases. Our Resileint Health team Osteopaths and Chiropractors tailor to your specific needs and can work with you in a variety of ways.
You can book in to see one of our practitioners
(CLICK the book online button in the top right corner ;) )
If you want more self care tips following a low back tweak, please check out the links below from world class Physiotherapist Dr Kelly Starrett from “The Ready State”
WHAT DO I DO IF BACK TWEAK:
LOW BACK TWEAK FAST FIXES:
References:
1. Dubois, B., & Esculier, J.-F. (2019). Soft-tissue injuries simply need PEACE and LOVE. British Journal of Sports Medicine, bjsports–2019–101253. doi:10.1136/bjsports-2019-101253
2. Liebenson, C. Rehabilitation of the Spine, 3rd Edition, Ch 2, Pg 63-64, Table 2.2